Tell your doctor straight away if you:have more than 2 of the common side effects – it means you could have too much digoxin in your blood. have a fast heart rate (palpitations), shortness of breath, feel dizzy or lightheaded and are sweating.
Common Side effects of Digoxin include:
- Dizziness.
- Mental disturbances.
- Diarrhea.
- Headache.
- Nausea.
- Vomiting.
- Red, bumpy rash.
Other medications can affect the removal of digoxin from your body, which may affect how digoxin works. Examples include azole antifungals (such as itraconazole), dronedarone, lapatinib, macrolide antibiotics (such as clarithromycin, erythromycin), propafenone, rifampin, St. John's wort, among others.
During digoxin treatment, the serum potassium concentration increased by 0.19 +/- 0.23 mmol(l)-1 (p < 0.05) during the period of rest. Thus, a digitalis-induced depression of Na-K-ATPase activity seems to be a prerequisite for the described change in serum potassium concentration.
Check your pulse before you take your digoxin. If your pulse is under 60 beats per minute, wait 5 minutes. Then check your pulse again. If it's still under 60, call your healthcare provider.
A low level of potassium in the body can increase the risk of digitalis toxicity. Digitalis toxicity may also develop in people who take digoxin and have a low level of magnesium in their body.
Digoxin remains one of the most frequently prescribed drugs in the management of atrial fibrillation. The main indications for digoxin in atrial fibrillation are restoration of sinus rhythm, prevention of recurrence and slowing of the ventricular rate.
Digoxin efficacy did not differ by level of GFR (P = 0.19 for interaction). Renal dysfunction is strongly associated with mortality in stable outpatients with heart failure, notably in patients with estimated GFR <50 ml/min per 1.73 m(2). The effect of digoxin did not differ by level of renal function.
Digoxin, also called digitalis, helps an injured or weakened heart pump more efficiently. It strengthens the force of the heart muscle's contractions, helps restore a normal, steady heart rhythm, and improves blood circulation. Digoxin is one of several medications used to treat the symptoms of heart failure.
In the case of severe digoxin intoxication, an antidote digoxin immune Fab (Digibind) is available. Digibind binds and inactivates digoxin.
Conclusions: Digoxin significantly decreases diastolic blood pressure during overnight sleep in patients with congestive heart failure. This effect is likely to be caused by reduction of sympathetic activity or increase of parasympathetic activity.
Digoxin is a cardiac glycoside and metoprolol is a beta-blocker. Side effects of digoxin and metoprolol that are similar include nausea and diarrhea.
Thiazide diuretics block the thiazide-sensitive NaCl transporter in the distal convoluted tubule, and can decrease calcium excretion.
Side effects include nausea, vomiting, diarrhoea, tiredness, insomnia, visual disturbances, palpitations and fainting. In rare cases, increased levels of digoxin in your blood can cause heart rhythm disturbances (arrhythmias). These are serious and require treatment as soon as possible.
The use of digoxin is limited because the drug has a narrow therapeutic index and requires close monitoring. Digoxin can cause many adverse events, is involved in multiple drug interactions, and can result in toxicity. Despite its limitations, however, digoxin has a place in therapy.
Overall, a meta-analysis of 11 observational studies by Ouyang et al (2015), including the AFFIRM Trial and TREAT-AF studies, found digoxin use was associated with greater risk for mortality in patients with AF, regardless of concomitant heart failure.
Although the direct effect of digoxin on blood vessels is vasoconstriction, when given to patients in heart failure, the systemic vascular resistance falls.
The mechanism by which digoxin or digitalis might cause liver injury is unknown. Digoxin is minimally metabolized in the liver and does not materially affect the activity of cytochrome P450 enzymes.
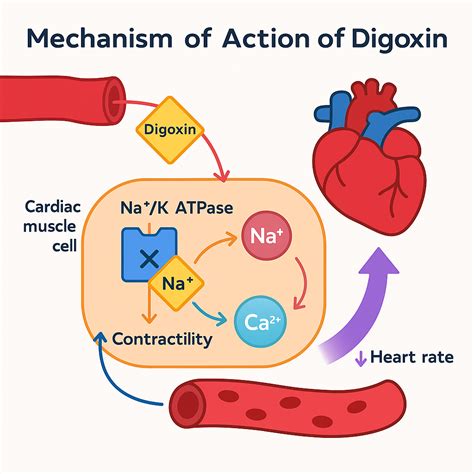
Digoxin exhibits its therapeutic and toxic effects by poisoning the sodium-potassium ATPase. The subsequent increase in intracellular sodium leads to increased intracellular calcium by decreasing calcium expulsion through the sodium-calcium, cation exchanger.
Erythromycin, clarithromycin, and tetracyclines - May increase digoxin levels. Propafenone - Increases digoxin level; effects are variable. Quinidine - Increases digoxin level substantially but clinical effect is variable; related drugs, such as hydroxychloroquine and quinine, may also affect levels.
Because digoxin binds to the K+ site of the Na+/K+-ATPase pump, low serum potassium levels increase the risk of digoxin toxicity. Conversely, hyperkalemia diminishes digoxin's effectiveness.
Therapeutic levels of digoxin are 0.8-2.0 ng/mL. The toxic level is >2.4 ng/mL.
Once distributed to the heart, digoxin binds to Na+/K+ ATPase pumps and inhibits their activity (see the figure). This causes the intracellular or cytosolic Na+ concentration to remain higher, which in turn disrupts the Na+ gradient needed to operate the Na+/ Ca2+exchange pump.
digoxin calcium gluconateAsk your doctor before using digoxin together with calcium gluconate. Taking these drugs together can affect the rhythm of your heart. Call your doctor if you have symptoms of irregular heartbeat, chest tightness, blurred vision, nausea, and seizures.
Digoxin belongs to the class of medicines called digitalis glycosides. It is used to improve the strength and efficiency of the heart, or to control the rate and rhythm of the heartbeat.
What is digoxin toxicity? Digoxin toxicity happens when you have too much digoxin in your body and it becomes harmful. Digoxin is a medicine that is used to treat heart failure or arrhythmias (abnormal heart rhythms). Digoxin toxicity can be life-threatening.
Therapeutic options range from simply discontinuing digoxin therapy for stable patients with chronic toxicity to digoxin Fab fragments, cardiac pacing, antiarrhythmic drugs, magnesium, and hemodialysis for severe acute toxicity.
Digitalis medicines strengthen the force of the heartbeat by increasing the amount of calcium in the heart's cells. (Calcium stimulates the heartbeat.) When the medicine reaches the heart muscle, it binds to sodium and potassium receptors.
Digoxin is primarily eliminated by the kidney. Patients with renal impairment may be at increased risk for digoxin toxicity, including ventricular arrhythmias and AV conduction disturbances, due to decreased drug clearance. Therapy with digoxin should be administered cautiously in patients with impaired renal function.
Magnesium improves the efficacy of digoxin in slowing the ventricular response in atrial fibrillation. Digoxin reduces tubular magnesium reabsorption, and in patients with congestive heart failure this interaction may be cumulative with other causes of magnesium deficiency (diuretics, diet, poor intestinal absorption).
In order to maintain a normal calcium level, the body uses hormones to regulate blood calcium levels. The normal regulation of calcium in our blood stream is similar to the way a thermostat works. The body is set to have a normal amount of calcium (somewhere between 8.6 to 10.3 mg/dL).
than in matched normal subjects (1.93 mEq./L.). These observations, coupled with the fact that both digitalis and magnesium deficiency lead to a decrease in intracellular potassium, suggested that hypomagnesemia might contribute to the development of digitalis toxicity.